Introduction: Why Your Gut Matters More Than You Think
The Complete Guide to Gut Health: Science-Based Insights for Optimal Wellness

Your gut is far more than a simple digestive tube. Often called the “second brain,” your gastrointestinal system houses approximately 100 trillion microorganisms—collectively known as the gut microbiome—that profoundly influence nearly every aspect of your health. From immune function to mental health, metabolic regulation to disease prevention, the health of your gut plays a central role in your overall wellbeing.
The past decade has witnessed an explosion of scientific research revealing the intricate connections between gut health and conditions ranging from obesity and diabetes to depression, autoimmune diseases, and even cancer. This comprehensive guide synthesizes the latest peer-reviewed research to provide you with evidence-based strategies for optimizing your gut health.
Part 1: Understanding Your Gut Microbiome
What Is the Gut Microbiome?
The gut microbiome refers to the complex ecosystem of bacteria, viruses, fungi, and other microorganisms living primarily in your large intestine. This microbial community contains approximately 1,000 different species of bacteria, with the four dominant phyla being Firmicutes, Bacteroidetes, Actinobacteria, and Proteobacteria.
Research from the NIH Human Microbiome Project has established that a healthy gut microbiome is characterized by high diversity—meaning a wide variety of different microbial species—and the right balance between beneficial and potentially harmful bacteria. This diversity appears to be crucial for maintaining health and preventing disease.
Key Functions of the Gut Microbiome
Your gut microbiome performs numerous critical functions:
Metabolic Functions: Gut bacteria break down complex carbohydrates and fibers that your body cannot digest on its own, producing short-chain fatty acids (SCFAs) like butyrate, propionate, and acetate. These SCFAs serve as fuel for your intestinal cells, help regulate metabolism, and have anti-inflammatory properties throughout your body.
Immune System Development and Regulation: Approximately 70-80% of your immune system resides in your gut. The microbiome trains your immune system to distinguish between harmful pathogens and benign substances, helping prevent both infections and autoimmune reactions.
Vitamin Synthesis: Certain gut bacteria produce essential vitamins including vitamin K, B vitamins (particularly B12, thiamine, and folate), which your body cannot produce on its own.
Protection Against Pathogens: Beneficial bacteria compete with harmful microorganisms for nutrients and space, produce antimicrobial compounds, and maintain the integrity of your intestinal barrier.
Neurotransmitter Production: Your gut bacteria produce or influence the production of neurotransmitters including serotonin, dopamine, and GABA, which affect mood, cognition, and behavior.
The Gut-Brain Axis
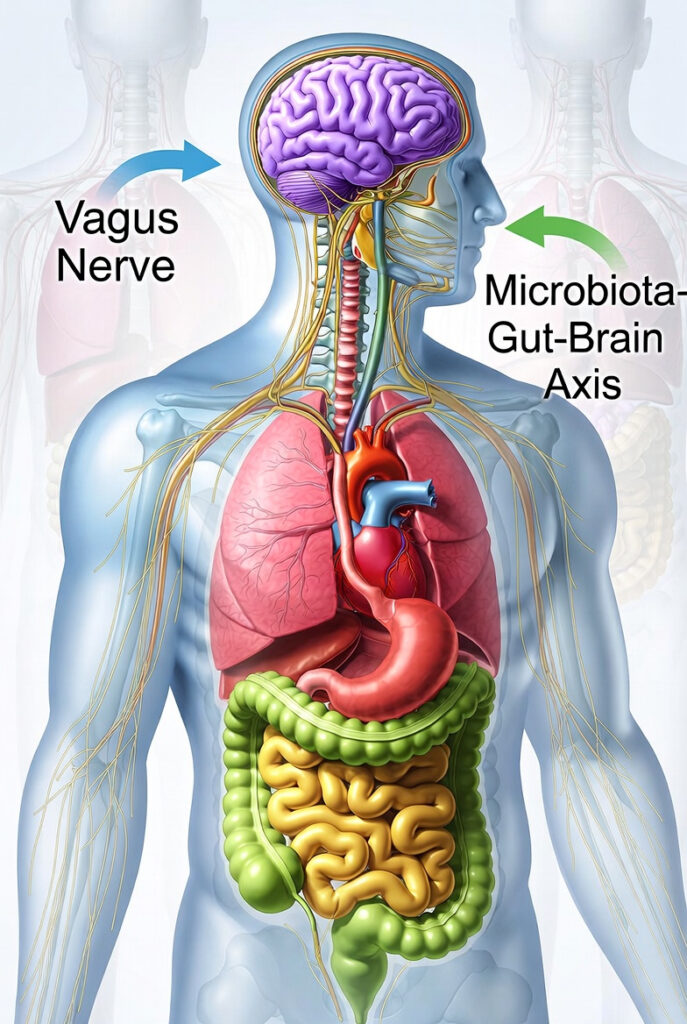
One of the most fascinating discoveries in recent years is the bidirectional communication pathway between your gut and brain, known as the gut-brain axis. This connection occurs through multiple channels:
- The Vagus Nerve: The longest cranial nerve that directly connects your gut to your brain
- Immune System Signaling: Inflammatory molecules produced in the gut can affect brain function
- Neurotransmitters: Gut bacteria produce neurotransmitters that influence mood and cognition
- Metabolites: SCFAs and other bacterial metabolites can cross the blood-brain barrier
Research has shown strong links between gut microbiome composition and mental health conditions including depression, anxiety, and even autism spectrum disorders. This has led to the emerging field of “psychobiotics”—probiotics that may have mental health benefits.
The Intestinal Barrier: Your Body’s First Line of Defense
Your intestinal lining is only one cell layer thick, yet it must perform the delicate task of allowing nutrients to pass through while keeping harmful substances, toxins, and pathogens out of your bloodstream. This selective permeability is maintained through:
- Tight Junctions: Protein complexes that seal the space between intestinal cells
- Mucus Layer: A protective gel coating produced by goblet cells
- Immune Cells: Specialized cells that monitor for threats
- Beneficial Bacteria: Microbes that strengthen the barrier and compete with pathogens
When this barrier becomes compromised—a condition sometimes called “intestinal permeability” or colloquially “leaky gut”—larger molecules and bacterial components can enter the bloodstream, potentially triggering inflammation and immune responses throughout the body.
Part 2: Health Implications of Gut Dysbiosis
What Is Dysbiosis?
Dysbiosis refers to an imbalance in your gut microbiome, characterized by:
- Loss of microbial diversity
- Overgrowth of potentially harmful bacteria
- Loss of beneficial bacteria
- Loss of overall microbial functions
Research has linked gut dysbiosis to numerous health conditions:
Metabolic Disorders
3. Artificial Sweeteners
Multiple studies have shown that artificial sweeteners like saccharin, sucralose, and aspartame can alter gut microbiome composition, reduce beneficial bacteria, and impair glucose metabolism—ironically, potentially contributing to the very metabolic problems they’re meant to prevent.
4. Chronic Stress
The gut-brain axis works both ways. Chronic psychological stress can alter gut microbiome composition, increase intestinal permeability, and promote dysbiosis through stress hormones and inflammatory pathways.
5. Sleep Deprivation
Poor sleep quality and insufficient sleep duration have been shown to alter gut microbiome composition, reduce beneficial bacteria, and increase markers of inflammation.
6. Excessive Alcohol Consumption
Excessive alcohol damages the intestinal barrier, promotes dysbiosis, allows bacterial components to enter the bloodstream, and triggers systemic inflammation.
7. Sedentary Lifestyle
Physical inactivity is associated with reduced microbial diversity. Exercise, conversely, promotes beneficial bacterial growth and microbiome diversity independent of diet.
8. NSAIDs and Proton Pump Inhibitors
Chronic use of non-steroidal anti-inflammatory drugs (NSAIDs) and proton pump inhibitors (PPIs) can damage the intestinal barrier, alter stomach and gut pH, and promote dysbiosis.
Part 4: Evidence-Based Strategies to Improve Gut Health
1. Dietary Fiber: The Foundation of Gut Health
Dietary fiber is the single most important nutritional factor for gut health. Fiber serves as food (prebiotic) for beneficial gut bacteria, which ferment it into short-chain fatty acids (SCFAs). Most adults should aim for 25-38 grams of fiber daily from diverse sources:
- Vegetables (especially cruciferous vegetables, leafy greens, onions, garlic)
- Fruits (especially berries, apples with skin, pears, bananas)
- Whole grains (oats, quinoa, brown rice, barley, farro)
- Legumes (beans, lentils, chickpeas, peas)
- Nuts and seeds (almonds, chia seeds, flaxseeds)
Research consistently shows that higher fiber intake is associated with increased microbial diversity, better metabolic health, reduced inflammation, and lower risk of chronic diseases.
2. Fermented Foods: Nature’s Probiotics

Fermented foods contain live beneficial bacteria and have been consumed for thousands of years across cultures. Recent research shows remarkable benefits:
Key Fermented Foods:
- Yogurt with live active cultures (look for Lactobacillus and Bifidobacterium strains)
- Kefir (fermented milk drink with diverse bacterial strains)
- Sauerkraut (unpasteurized – pasteurization kills beneficial bacteria)
- Kimchi (Korean fermented vegetables)
- Kombucha (fermented tea)
- Miso (fermented soybean paste)
- Tempeh (fermented soybeans)
- Traditional pickles (naturally fermented, not vinegar-based)
A landmark Stanford study published in 2021 found that consuming 6 servings of fermented foods daily for 10 weeks significantly increased microbiome diversity and decreased 19 inflammatory markers, including interleukin-6.
3. Probiotics and Prebiotics
Probiotics are live beneficial bacteria that can colonize your gut, while prebiotics are fibers that feed these bacteria. The combination of both (called synbiotics) can be particularly effective.
Proven Probiotic Strains:
- Lactobacillus acidophilus: Supports digestion and immune function
- Bifidobacterium longum: Reduces inflammation and supports gut barrier
- Lactobacillus rhamnosus GG: Prevents antibiotic-associated diarrhea
- Saccharomyces boulardii: A beneficial yeast that fights pathogens
- Bifidobacterium bifidum: Supports immune system development
Prebiotic Foods:
- Garlic and onions
- Leeks and asparagus
- Jerusalem artichokes
- Chicory root
- Bananas (especially slightly green)
- Oats and barley
When choosing probiotic supplements, look for products with:
- Multiple strains (diversity is beneficial)
- At least 1 billion CFUs (colony-forming units)
- Strains with research backing for your specific needs
- Proper storage (refrigeration when required)
4. Polyphenol-Rich Foods
Polyphenols are plant compounds with antioxidant properties that also serve as fuel for beneficial gut bacteria. They can increase the growth of helpful bacteria while suppressing harmful ones.
Top Polyphenol Sources:
- Green tea and matcha
- Dark chocolate (70%+ cacao content)
- Berries (blueberries, blackberries, strawberries)
- Red wine (in moderation – 1 glass for women, 1-2 for men)
- Extra virgin olive oil
- Coffee
- Nuts (especially walnuts, pecans, hazelnuts)
- Colorful vegetables (red cabbage, artichokes)
5. Regular Physical Exercise
Exercise is a powerful modulator of the gut microbiome. Studies show that regular physical activity increases microbial diversity and promotes beneficial bacteria independent of diet.
Exercise Benefits for Gut Health:
- Increases production of SCFAs
- Enhances gut barrier function
- Reduces gut inflammation
- Promotes growth of butyrate-producing bacteria
- Improves gut motility
Recommendations:
- Aim for at least 150 minutes of moderate-intensity aerobic activity weekly
- Include resistance training 2-3 times per week
- Incorporate movement throughout the day (walking, stretching)
- Find activities you enjoy for long-term adherence
6. Stress Management Techniques
Chronic stress directly impacts gut health through the gut-brain axis. Implementing stress reduction strategies can significantly improve gut function.
Proven Stress Reduction Methods:
- Meditation and Mindfulness: Even 10 minutes daily can reduce stress hormones
- Yoga: Combines movement with breath work and stress reduction
- Deep Breathing Exercises: Activates parasympathetic nervous system
- Regular Social Connection: Strong relationships buffer against stress
- Time in Nature: Forest bathing and outdoor activities reduce cortisol
- Cognitive Behavioral Therapy: Addresses negative thought patterns
- Journaling: Helps process emotions and reduce rumination
7. Prioritize Quality Sleep
Sleep and gut health have a bidirectional relationship – poor sleep harms your microbiome, and an unhealthy gut disrupts sleep. Aim for 7-9 hours nightly.
Sleep Hygiene Strategies:
- Consistent sleep schedule
- Cool, dark bedroom (65-68°F)
- Limit screens 1-2 hours before bed
- Avoid late meals, caffeine, alcohol
- Morning sunlight exposure
8. Stay Hydrated
Water supports the intestinal mucosal lining and bacterial balance. Aim for 8-10 glasses daily.
9. Targeted Supplements
While food is primary, consider: L-Glutamine, Zinc, Vitamin D, Omega-3s. Consult healthcare provider first.
Part 5: Practical Action Plan
Phase 1: Foundation (Weeks 1-4)
- Gradually increase fiber to 30+ grams daily
- Add one fermented food daily
- Reduce ultra-processed foods
- Drink 8-10 glasses water
- Sleep 7-9 hours consistently
- Move 20-30 minutes daily
Phase 2: Building (Weeks 5-12)
- Diversify fiber – 30+ plant foods weekly
- Try 2-3 fermented foods
- Add polyphenol-rich foods daily
- Practice stress management 10+ minutes
- Exercise 150 minutes weekly
- Consider quality probiotic
Phase 3: Maintenance (Month 3+)
- Make gut-friendly eating automatic
- Maintain diverse plant diet
- Continue exercise routine
- Practice ongoing stress management
- Annual gut health check-ins
Signs of Improvement (2-12 weeks):
- Regular bowel movements
- Reduced bloating
- Better energy and mood
- Improved sleep quality
- Fewer illnesses
- Clearer skin
When to Seek Help:
- Persistent digestive issues > 2 weeks
- Unintended weight changes
- Blood in stool
- Severe symptoms despite changes
Conclusion
Your gut microbiome is remarkably responsive to positive changes. Even small, consistent improvements yield significant benefits within weeks. Start with the foundational changes – particularly fiber, fermented foods, and reducing processed foods.
Key Takeaways:
- Fiber is fundamental – 30+ grams daily
- Fermented foods are powerful
- Diversity matters – 30+ plant foods weekly
- Lifestyle factors crucial – sleep, stress, exercise
- Avoid gut disruptors
- Be patient and consistent
- Individualize your approach
By prioritizing gut health today, you’re investing in long-term wellbeing and disease prevention. Start your journey now – your gut will thank you.
Disclaimer: This is for informational purposes only, not medical advice. Consult healthcare professionals before significant diet, lifestyle, or supplement changes, especially with existing conditions or medications.
